Browse Tag
IVF Specialist in Bangalore
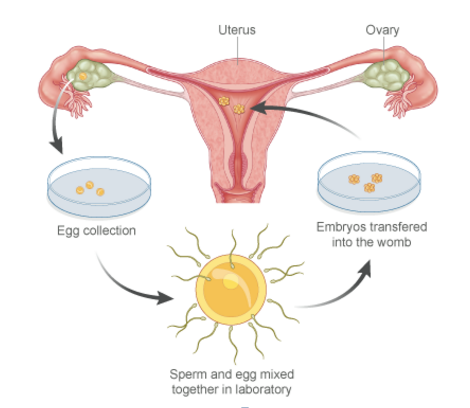
Does the collection of eggs increase the chance of pregnancy from IVF?
The process of IVF(In-Vitro-Fertilization) involves the ovarian stimulation with hormones with the intention of retrieving more eggs. The whole idea is to have enough eggs to produce an optimum number of good embryos to transfer and to freeze a few in case the fresh transfer fails. The question here is how many do we actually need? What is the optimum number of eggs needed to achieve a live birth, which in turn is the ultimate aim of IVF?