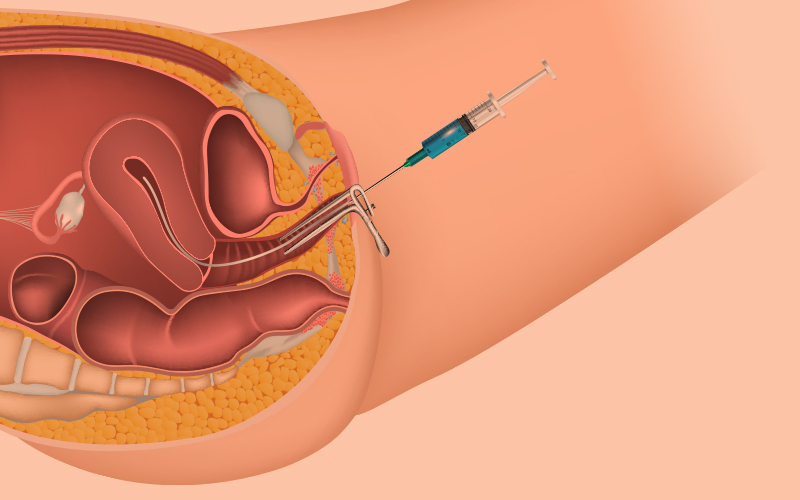
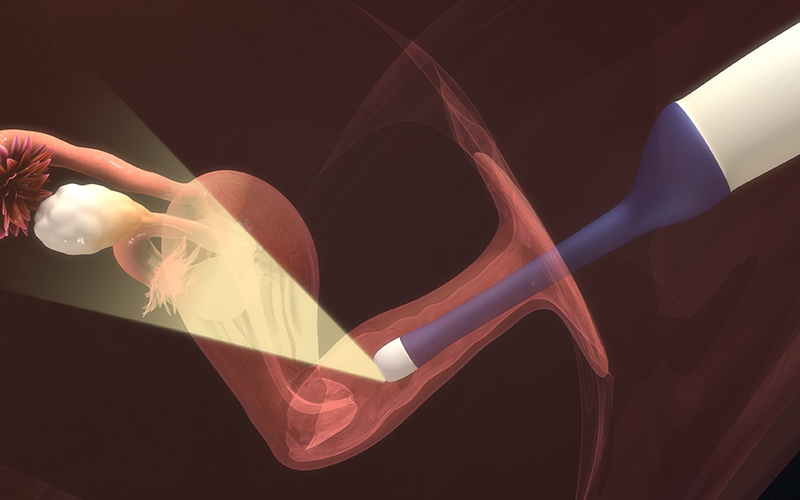
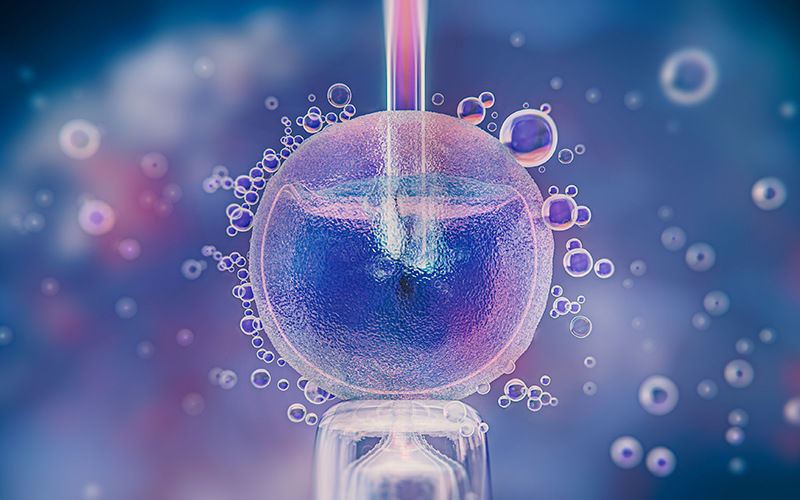
Polycystic ovarian syndrome (PCOS) is a health condition that affects women of childbearing age.
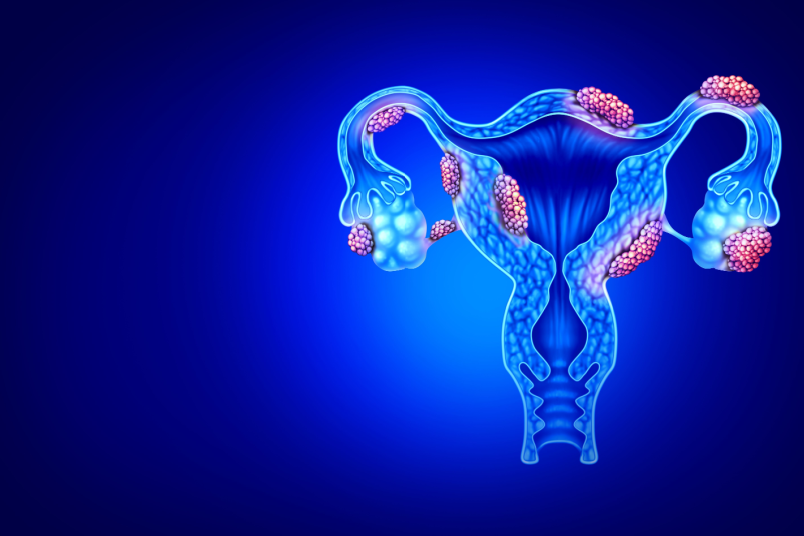
In this condition, the ovaries tend to produce excess androgens, a male sex hormone that is usually present in small amounts in women. The name, polycystic ovarian syndrome, describes numerous small cysts (fluid-filled sacs) in the ovaries.
However, these are different from the other ovarian cysts which require surgery. PCOS can have an impact on a woman’s overall health as well as their physical appearance. Although common, PCOS is often a treatable condition.